by Marco Gontijo
Tuberculosis (TB) is history’s deadliest infectious disease, responsible for over a billion deaths in the past two centuries. Yet, it rarely makes headlines today. Unlike COVID-19 or Ebola, which triggered immediate public concern, TB has faded from attention due to medical advancements, shifting public perception, and changing global health priorities.
Mycobacterium tuberculosis, the causative agent of TB, enters the lungs when a person inhales infected droplets (Figure 1). The bacteria infect immune cells called alveolar macrophages, which try to contain the infection by forming a granuloma protective cluster. You can think of this like a fortress that the immune cells build around the infection, trapping the bacteria inside to prevent them from spreading further. If the immune system is strong, the infection stays latent, meaning the person carries the bacteria without symptoms. However, if the immune system is weakened, the bacteria can escape, leading to active TB disease, which triggers symptoms like coughing and lung damage. Granulomas sometimes break down (necrosis), releasing bacteria that can spread to parts of the body. People with latent TB are not entirely safe either, as they may later develop active disease if their immune defenses weaken. Factors that can weaken the immune system include conditions like HIV/AIDS, malnutrition, aging, immunosuppressive treatments (e.g., corticosteroids or chemotherapy), and certain chronic illnesses like diabetes.
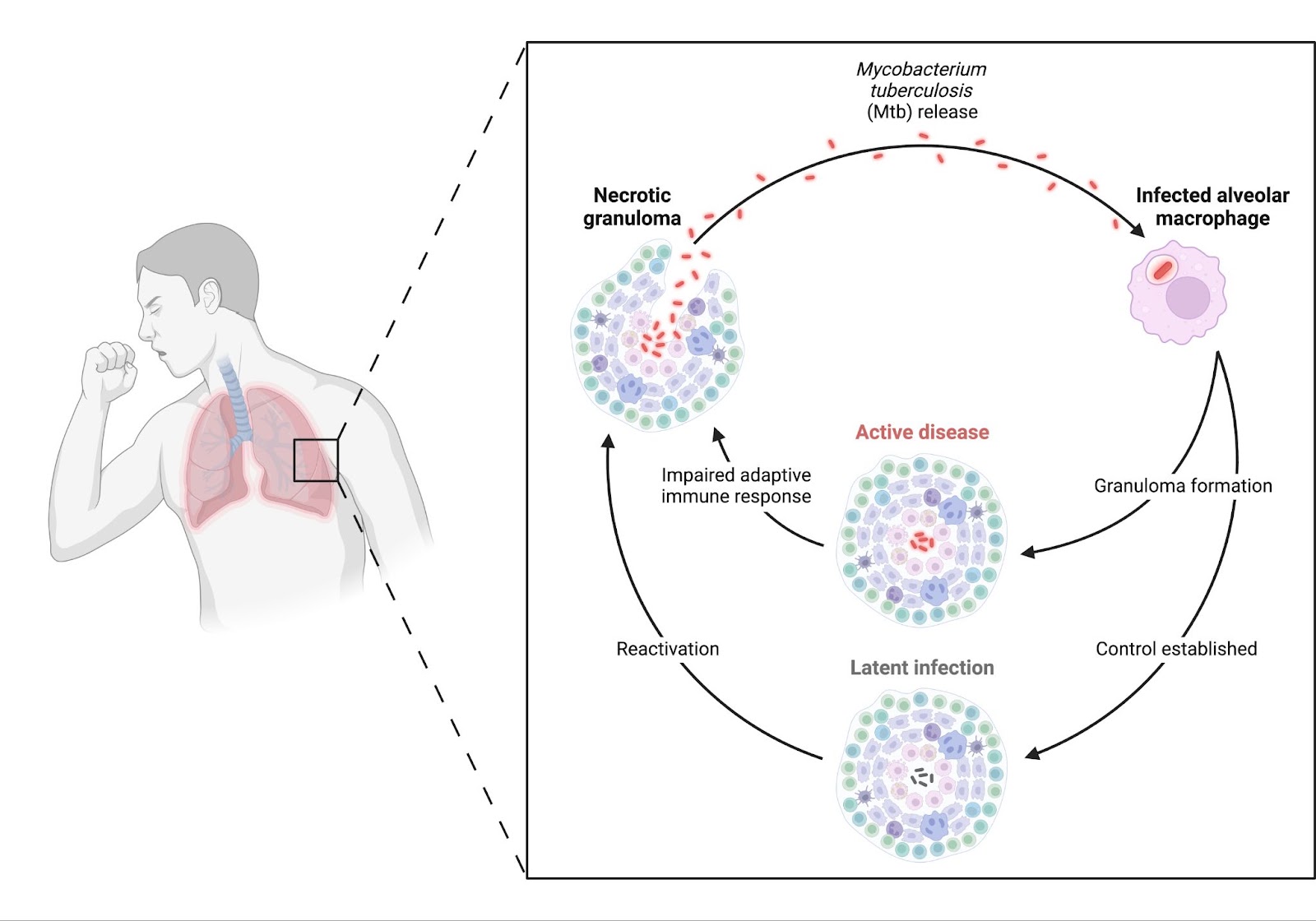
Figure 1. How TB develops and spreads in the body. (Image generated by author in BioRender)
A Disease of the Past?
TB is often seen as a disease of the past, once a significant public health crisis in the 19th and early 20th centuries. The introduction of antibiotics like streptomycin and isoniazid in the mid-20th century drastically reduced cases in wealthier countries, leading to a decline in public awareness. However, TB remains a global threat, still killing over a million people annually, mostly in low- and middle-income countries. The rise of drug-resistant strains further complicates efforts to control the disease, yet in regions where TB is no longer common, it is largely forgotten.
The “Silent” Pandemic
TB lacks the urgency of diseases like COVID-19 or Zika because it progresses slowly and doesn’t cause sudden outbreaks. The bacterium Mycobacterium tuberculosis can remain dormant for years, with most latent infections never becoming active, reducing its shock factor. Additionally, TB primarily affects marginalized populations—those in poverty, with limited healthcare, or compromised immune systems—who have less political influence, leading to minimal public pressure for action.
Competing Health Priorities
Public health efforts often focus on immediate crises. During COVID-19, resources were redirected, disrupting TB programs and increasing TB-related deaths. With limited funding, global health organizations prioritize urgent threats. TB control requires long-term strategies like vaccination, antibiotics, and improved living conditions, which lack the dramatic urgency needed to sustain public and political interest.
Can TB Regain the Spotlight?
Although TB is not a “new” disease, recent Kansas and North Carolina outbreaks highlight the need for renewed attention. The Kansas outbreak, with 67 cases and two fatalities, underscores vulnerabilities in public health infrastructure. In contrast, the North Carolina outbreak revealed a rare, bone-infecting strain, resembling an ancestral form of TB.
These outbreaks were primarily triggered by increased migration, crowded living conditions, and, in some cases, delays in diagnosing or treating TB. Given that TB remains a threat, especially in high-risk areas with poor healthcare access, similar outbreaks could continue to occur in other states if preventive measures are not strengthened. This emphasizes the importance of vigilance and timely intervention to prevent the spread of TB, especially as many people believe it is no longer a significant concern.
These cases demonstrate that TB is far from eradicated and continues to evolve. Advances in diagnostics, shorter treatment regimens, and new vaccines could transform TB control, but achieving the WHO’s goal of global TB elimination by 2035 requires sustained awareness and funding. Public health campaigns, media coverage, and advocacy are essential to keeping TB a priority. The lessons learned from COVID-19—rapid response, global collaboration, and vaccine development—can be applied to TB, but only if the world recognizes it as an ongoing and urgent challenge. Without action, TB will continue to threaten millions worldwide.
