by Hannah Thrash
Macrophages are one of my favorite immune cells. These little guys are found throughout the body and act as guards against all kinds of pathogens. When they detect a threat, they eat it (literally) in a process called phagocytosis, protecting the body and defeating the pathogen. While we know what macrophages do to invaders from outside the body, such as bacteria and viruses, scientists are interested in learning what they do to threats from within the body, such as cancer.
One of the most interesting things that scientists have uncovered about cancer-associated macrophages is that there are two distinct types, and they have two different functions (Figure 1). These two types of macrophages are shaped by the environments they come from and, based on this external influence, have opposing roles in cancer. M1 Macrophages are tumor-fighting macrophages. These immune cells have specific receptors, such as those shown in Figure 1, and when these receptors receive chemical signals from the cancer cells around them, that activates anti-tumor transcription factors and pathways within the macrophage. They then release anti-tumor factors directly into the tumor itself! M2 macrophages, on the other hand, are tumor-supporting macrophages. These cells have pro-tumor receptors that turn on pathways and lead to the production of factors, such as cytokines and hormones, that help support tumor formation and progression.
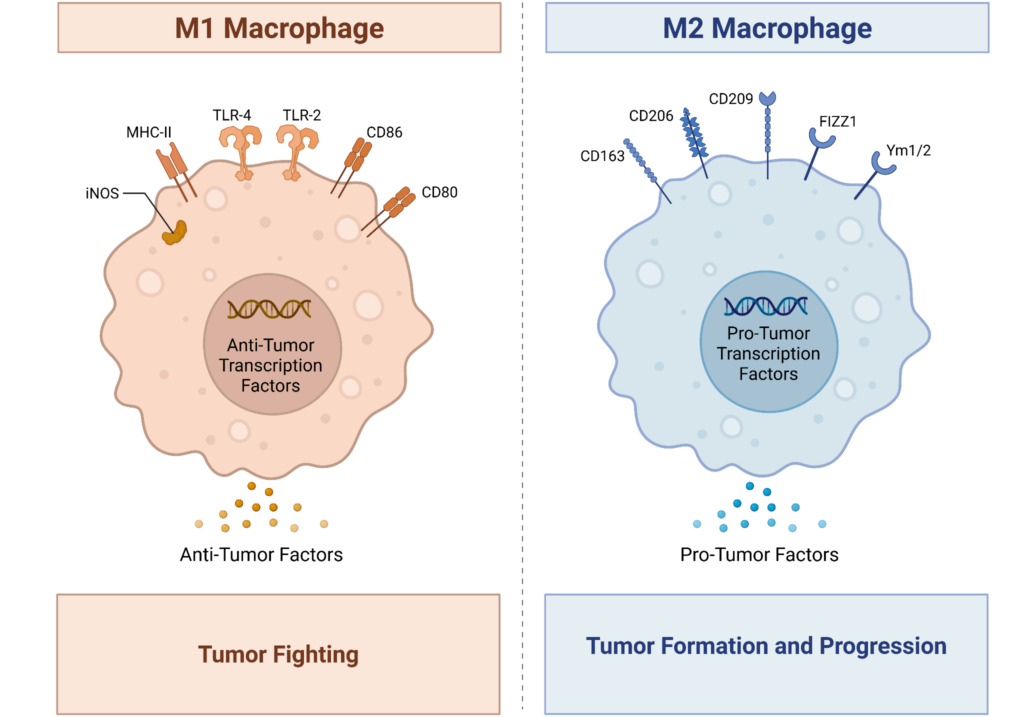
Figure 1: Cancer-associated macrophages. M1 macrophages (left, orange) have specific receptors (iNOS, MHC-II, TLR-4, TLR-2, CD86, CD80) that turn on anti-tumor transcription factors and cause the macrophage to act in an anti-tumor function by secreting anti-tumor factors. These macrophages are tumor-fighting. M2 macrophages(right, blue) have a completely different set of receptors (CD163, CD206, CD209, FIZZ1, Ym1/2). These receptors activate pro-tumor transcription factors, causing the macrophage to release pro-tumor factors. These macrophages help promote tumor formation and progression. (Image created in Biorender by the author using a template deposited in Biorender by Yao, Y., Xu, X. H., & Jin, L. (2019). Macrophage Polarization in Physiological and Pathological Pregnancy. Frontiers in immunology, 10, 792. https://doi.org/10.3389/fimmu.2019.00792).
The question researchers want to answer is: how can we keep M1 anti-tumor macrophages within the tumor, killing it from within via their anti-tumor factors, while keeping out M2 pro-tumor macrophages? Initially, this problem was very difficult for researchers. M1 and M2 macrophages share many similarities and have the same cell of origin, meaning they start as the same cell type before transforming into the two distinct types. However, researchers then realized that the key to targeting different cells lies in differences in their receptors. Looking back at Figure 1, M1 macrophages express receptors such as iNOS, MHC-II, TLR-4, TLR-2, CD86, and CD80, while M2 macrophages express receptors including CD163, CD206, CD209, FIZZ1, and Ym1/2. Notice that there is no overlap in these lists! So, in order to target just M2 macrophages, scientists use drugs and identification systems that look for the receptors specific to just the M2 macrophages. This way, we can keep the good (M1) macrophages while keeping out the bad (M2) and promote tumor-fighting by the body’s own immune system!
